In our last post we looked at the mysterious new form of hepatitis affecting young children. But what about hepatitis B and hepatitis C, which are already well known problems for thousands of Australians? How do they affect children?
Occurrence
Hepatitis B isn’t common in young Australians because children born here are routinely immunised against it as part of the National Immunisation Program. The first of four free vaccination shots is usually given within a week of birth, with the others following at 2, 4 and 6 months of age (often in combination with other vaccinations). Babies who are born very prematurely or have a low birth weight get an additional free hepatitis B vaccine at 12 months.

If a pregnant woman has hepatitis B, she is usually given medicine to reduce the chance of passing the virus on to her baby. At birth, the baby might also get a extra injection of antibodies against hepatitis B, given within the first 12 hours, as well as the standard hepatitis B immunisation. Women who have hepatitis B can safely breastfeed unless their nipples are cracked or bleeding, as the virus can be transmitted in blood.
Hepatitis C is also rare in Australian children, due to to the fact that is is usually quite hard to transmit: it can only happen when blood containing the virus enters another person’s bloodstream. Household contact could lead to this happening, for example if a child uses a toothbrush belonging to an adult living with hepatitis C, or if they receive a needle stick injury after finding injecting equipment belonging to an adult. There is also a small risk of transmission if the mother breastfeeds with cracked or bleeding nipples.

Transmission
What about the risks of transmitting viral hepatitis during pregnancy, birth or breastfeeding? In Australia, it is recommended that all pregnant women should be tested for hepatitis B and C. Testing in pregnancy allows arrangements to be made for vaccinating the newborn if the mother is found to have hepatitis B, or for precautions to be taken to prevent transmission of hepatitis C to the baby after birth. If a pregnant woman is found to have hepatitis C, plans can also be set up for her to start treatment once she is no longer breastfeeding. If hepatitis testing has not taken place for some reason, hepatitis C testing of pregnant women who are to have a planned invasive procedure — such as a Chorionic villus sampling (CVS) — has also been recommended, due to the small risk of blood-to-bloodstream hepatitis C transmission to the baby.
For hepatitis B, mother-to-child transmission can happen either in the uterus, through placental leakage, or through exposure to blood or blood-contaminated fluids at or around the time of birth. Perinatal transmission (transmission which takes place during or soon after the time of birth) is believed to account for between a third and a half of all hepatitis B infections.
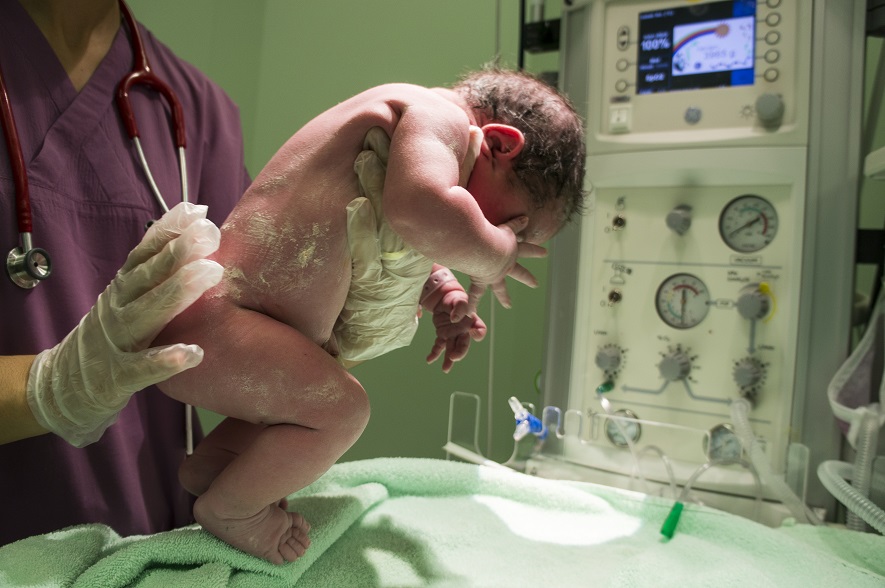
If a pregnant woman is living with hepatitis C, it is actually extremely unlikely that she will pass on the virus to her child in utero: the risk is less than 5%. The greatest risk during birth is if a medical intervention is needed: for example, forceps can scratch a child’s skin, allowing blood-borne transmission. If the mother is known to have hepatitis C, then any interventions can be adjusted with this in mind to reduce risk as much as possible. Identifying women who have hepatitis C during pregnancy means that interventions that increase the risk of transmission to the baby can be avoided and effective treatments commenced after the birth or cessation of breastfeeding.
Because children with hepatitis B often don’t have symptoms, transmission between children may easily occur during play or fight through cuts and scratches.
Treatment
If a child is living with viral hepatitis, what can be done? Clinical trials have recently shown that treatment of hepatitis C infection in children with the same medications used for those over the age of 18 is safe and effective, and these treatments have a cure rate of more than 97%.
Hepatitis C treatments listed on the Pharmaceutical Benefits Schedule can now be prescribed to children over three years old. However, they should be referred to a paediatrician who has experience with hepatitis C treatment, to discuss therapy options.
When children become infected with hepatitis B, some will recover from the virus within weeks or months without any medical intervention, and indeed may not even feel any effects from the infection. A majority (about 90%) of younger children who contract hepatitis B will develop chronic hepatitis B and will live with the virus long-term. This can put them at risk of liver scarring, liver failure and liver cancer in the future, so it is vital that children with chronic hepatitis B have liver and general health checks every 6-12 months depending on the advice of medical professionals. Although there is currently no cure for hepatitis B, there are some safe and effective anti-viral medicines to ameliorate its effects.
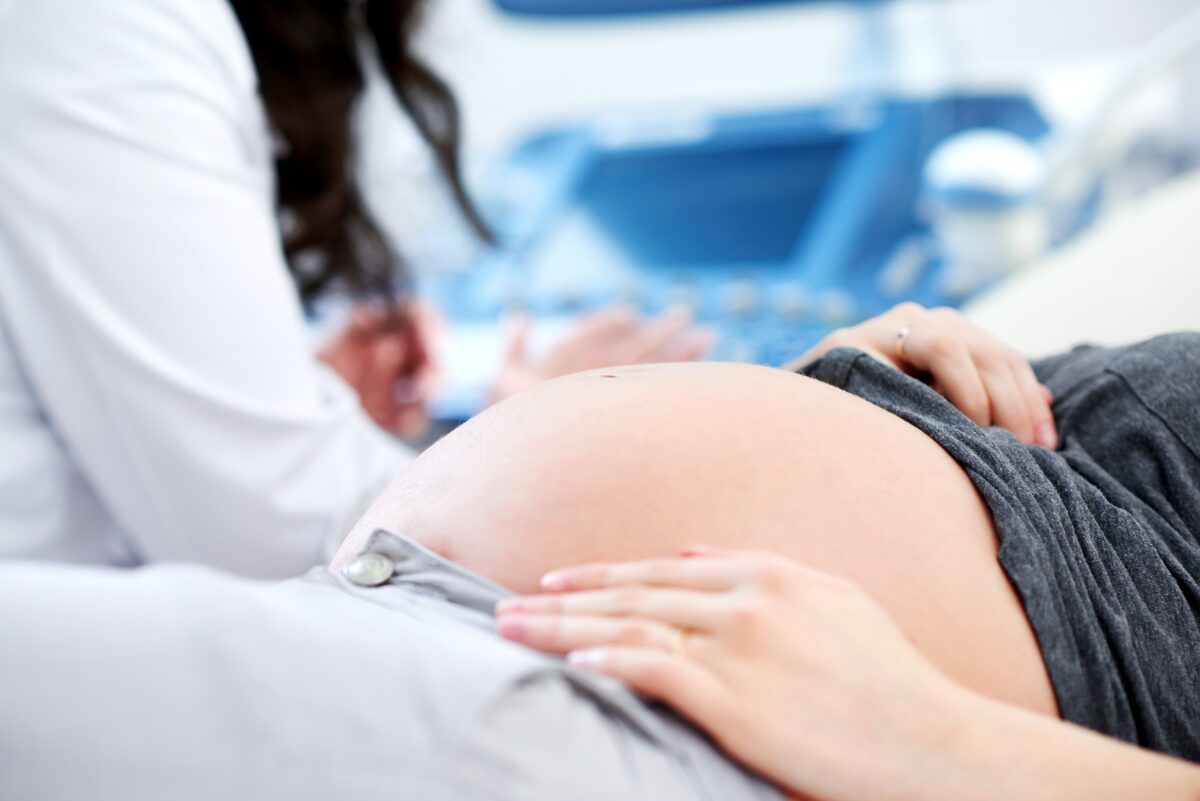
Any pregnant women or children living with viral hepatitis should be put in touch with a liver health nurse or specialist, in order to make sure that the best decisions are made for their health. It’s also extremely important to make all tests and services easily available for Aboriginal or Torres Strait women or women born overseas, as they are statistically more likely to have been exposed to viral hepatitis in the course of their lives.
If you have any concerns about your health or your child’s health, always remember to talk to your GP with any questions you might have, or you can call Hepatitis SA on 1800 437 222 or chat to us via the webchat icon at the bottom of our homepage.
Further reading:
https://www.schn.health.nsw.gov.au/fact-sheets/hepatitis-b-virus-infection-in-infants-and-children
https://www.schn.health.nsw.gov.au/fact-sheets/hepatitis-c-virus-infection-in-children
Last updated 10 April 2025
More from:
Enjoyed this article? Subscribe to be notified whenever we publish new stories.
Subscribe for Updates




