Scientists at Melbourne’s Doherty Institute are asking, “What if there was a way to predict which patients are more likely to achieve functional cure of chronic hepatitis B virus infection?” And they might have the answer.
A Doherty research study, funded by Gilead Sciences, a US-based pharmaceutical company, found that people living with a version of the hepatitis B virus (HBV) that is less genetically diverse are more likely to achieve functional cure on treatment.
“There is no cure for chronic hepatitis B but, on rare occasions, current antiviral treatment can achieve what we call ‘functional cure’ – that is the loss of hepatitis B surface antigen (HBsAg), a biomarker indicative of the virus in the blood,” explained the Royal Melbourne Hospital’s Professor Peter Revill, Head of Regional and Global Health in the Victorian Infectious Diseases Reference Laboratory (VIDRL) at the Doherty Institute.
“We wanted to know how likely a person with chronic hepatitis B is to reach functional cure during their antiviral therapy.”

[Image: Freepik/kjpargeter]
When the hepatitis B virus replicates itself in the body, it has no error correction system, and so can accidentally produce copies of itself with changed genetic information. It may end up producing many different variants of its original genetic code. A measurement known as a haplotype number (HN) quantifies this diversity: the lower the number, the less diverse the viral genome.
The team studied hepatitis B virus variants in people living with HBV to identify predictors of disease outcome and treatment response. The researchers found that a lower haplotype number (≤2) in a patient was associated with a higher chance to achieve functional cure on antiviral therapy.
“This is the first study to show that haplotype number at baseline predicts which patients may, or may not, achieve functional cure on current antiviral therapy,” said the Royal Melbourne Hospital’s Dr Josef Wagner, Senior Medical Scientist in the VIDRL, and lead author of the paper.
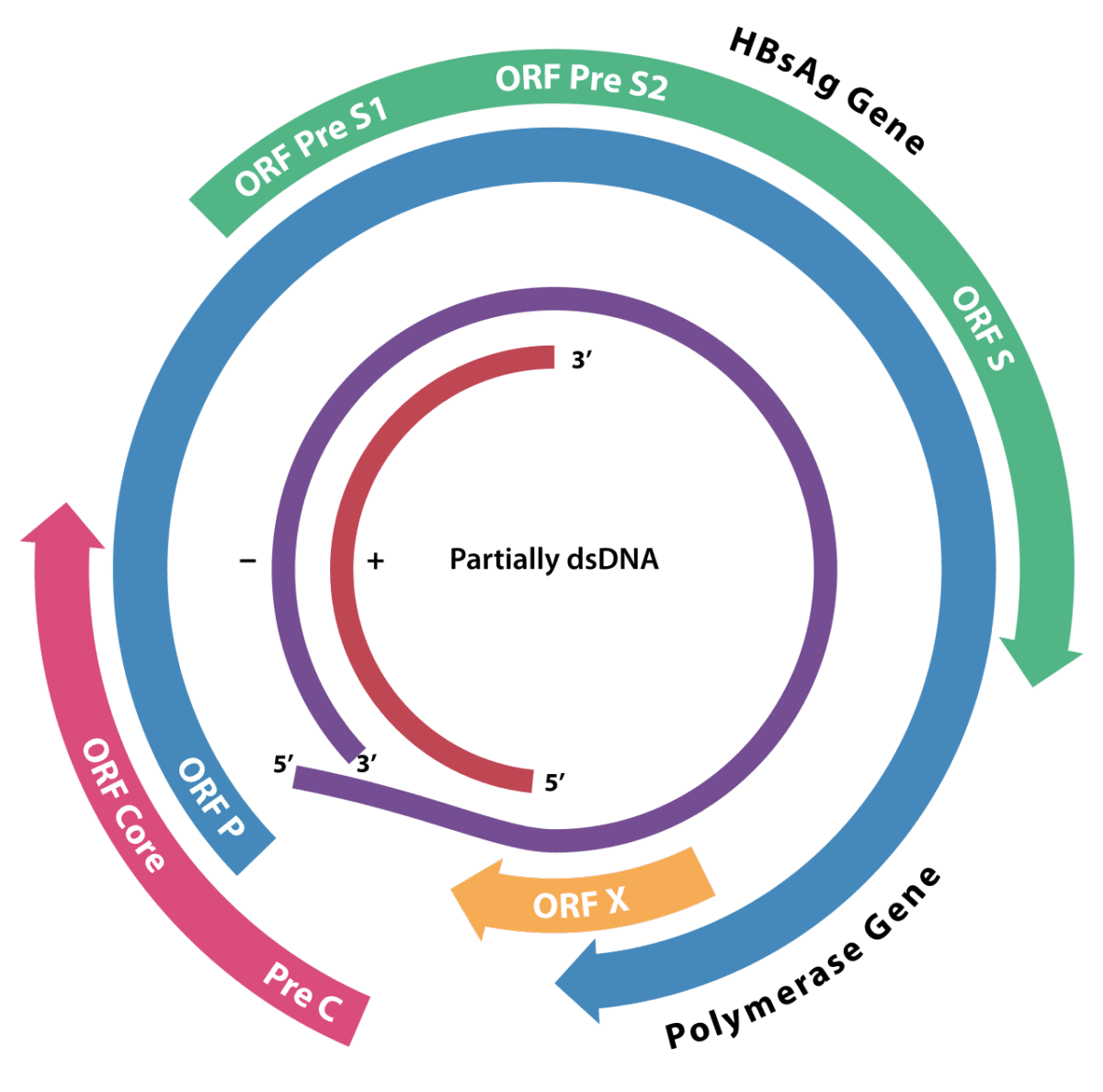
“At present our findings are limited to hepatitis B virus genotypes A and D, and further studies are required with additional HBV genotypes.”
The Royal Melbourne Hospital’s Dr Margaret Littlejohn, Senior Medical Scientist within the Molecular Research and Development laboratory at VIDRL, said that this is a great step in providing tools for clinicians to treat their patients more efficiently.
“For patients living with chronic hepatitis B, we can now establish the HBV haplotype population from a blood serum sample in a fast and efficient manner, predicting which patients may or may not achieve functional cure on treatment in some settings, thereby providing clinicians with an effective biomarker of treatment response.”
Last updated 24 April 2026
More from:
Enjoyed this article? Subscribe to be notified whenever we publish new stories.
Subscribe for Updates