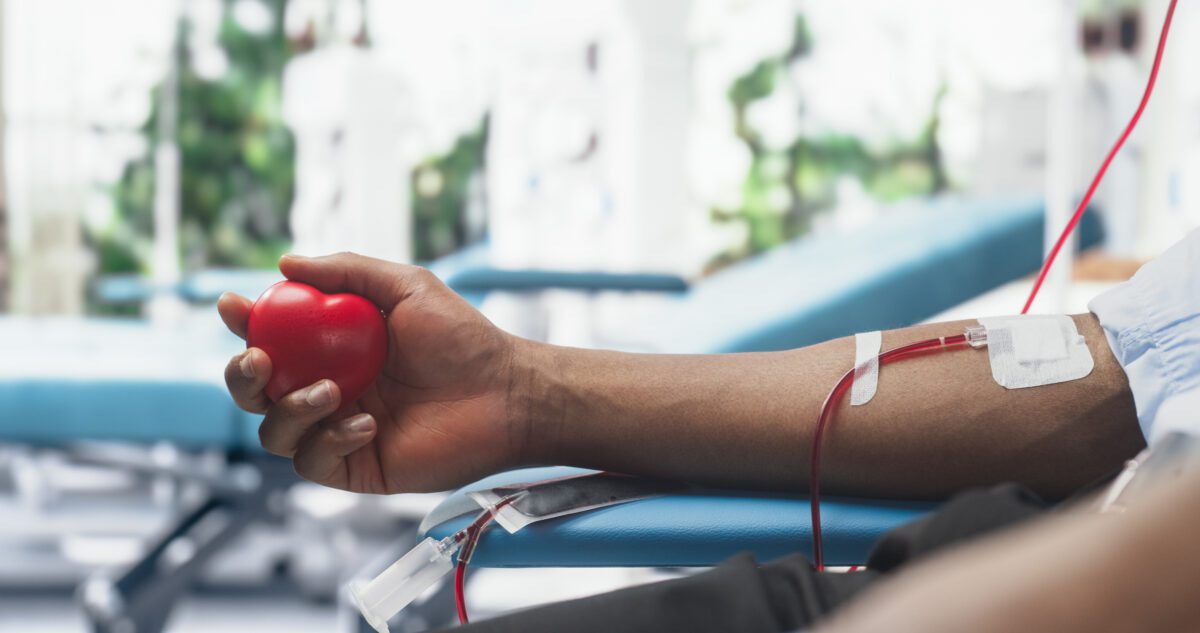
Opioid substitution treatment (OST) clinics are considered ideal locations for providing treatment for people with chronic hepatitis C virus infection who inject drugs, a vital priority group for achieving the goal of HCV elimination. But despite the availability of highly effective treatments with relatively few side effects, treatment uptake is yet to reach the level needed to achieve elimination.
Research led by Heidi Coupland, of Drug Health Services in the Sydney Local Health District, explored competing priorities among clients, clinic staff and policy makers, and the resulting barriers to beginning HCV treatment in OSTs.
Coupland’s team conducted in-depth interviews with clients and staff from two hospital-based opioid substitution treatment clinics in Sydney. The interviews were then thematically and rigorously analysed.
For the majority of clients—more than three quarters—HCV treatment was not a priority and many preferred to postpone treatment. Work and family obligations, health problems, focusing on drug treatment issues, and perceptions that HCV was an additional and unwanted commitment and responsibility, shaped clients’ decision-making. “I’ll have hep C treatment eventually,” was the overall theme.

Clients also identified concerns about side-effects and the barriers posed by the multiple steps involved in pre-treatment testing and getting scripts filled. Many clients (69%) reported that clinic staff strongly encouraged them to commence treatment, and they perceived staff to have a clear agenda during their interactions.
OST clinics are required to harness considerable resources to make testing and treatment more accessible for clients, given their existing staff capacity and both institutional and prescribing-related barriers. Data gathered from the interviews highlighted the need for adequate staff and appropriate record-keeping systems for capturing and storing relevant tracking data to facilitate client linkage to treatment, and for reporting progress.
The study found that eliminating HCV in Australia’’s resource-constrained OST settings requires a marked reorientation of the available resources. Given the disparities between the priorities of clients and staff regarding treatment uptake, real challenges persist in maintaining client-centred service provision for a population with multiple health and social needs.
Homelessness vs treatment
With liberal access to direct acting antivirals in Australia, and recommendations for all people living with HCV to be treated, most people accessing clinical services should be treated. A study led by Rosie Gilliver of the Kirketon Road Centre in Sydney’s Kings Cross describes a cohort of individuals aware of their HCV diagnosis but who have yet to initiate treatment despite its recommendation.

The results showed that clients receiving Opioid Substitution Treatment were no more likely to initiate treatment than those not receiving OST: 81% versus 77%. Those experiencing homelessness were significantly less likely to initiate treatment than those who were not homeless: 78% versus 89%. Those reporting recent injecting drug use were equally likely to initiate treatment as those reporting no recent use: 73% versus 69%.
Every Kirketon Road Centre client with detectable HCV RNA who was worked up for DAA therapy between March 2016 and March 2019 was included in the study, though clients known to have been treated at another service were excluded. Demographic, behavioural, attendance and clinical variables were factored into the results. Clients known to the service for less than a month prior to their HCV assessment were considered existing clients.
During the 3-year timeframe, 456 individuals were diagnosed and assessed for DAA treatment. Of these, 328 individuals commenced DAAs at Kirketon Road, with 128 clients remaining untreated. Overall treatment uptake was therefore 72%.
No other demographic factors, including gender, Aboriginality, or other variables such as attendance at outreach or main site locations or duration of relationship with the service were significantly associated with lower treatment uptake.
So, homelessness was shown to be the most notable factor in affecting the client’s going onto treatment. But it’s important to note that those clients who are housed and who attend Kirketon Road are still often highly socially disadvantaged, and it is clearly important that someone’s current housing status does not lead to an assumption of likely engagement in care.
Despite high overall treatment uptake, a significant proportion of clients remain untreated. Many still attend the service, but have not commenced treatment despite it being offered. Significant social instability compromised Kirketon Road’s capacity to work up and initiate treatment with these clients.

Last updated 24 May 2024
More from:
Enjoyed this article? Subscribe to be notified whenever we publish new stories.
Subscribe for Updates